Pericardiocentesis
is a crucial medical procedure employed to address pericardial effusion, an
accumulation of fluid in the pericardium, the sac enveloping the heart. This
condition, if left untreated, may lead to cardiac tamponade, a life-threatening
situation. Pericardiocentesis serves both diagnostic and therapeutic purposes,
offering relief from symptoms and preventing complications by draining excess
fluid, thereby reducing pressure on the heart.
Procedure Details: Pericardiocentesis is indicated when there
is a substantial buildup of fluid in the pericardial sac, a condition
associated with diverse causes such as infection, inflammation, trauma, or
cancer. It serves as a diagnostic tool to identify the underlying cause while
simultaneously acting as a therapeutic measure to relieve pressure on the
heart.
Procedure Steps:
1.
Patient Preparation: The patient is positioned appropriately, and the skin over the
pericardial area is thoroughly cleaned and sterilized to minimize the risk of
infection.
2.
Local Anesthesia: Before the procedure, a local anesthetic is administered to numb the
skin and underlying tissues, ensuring the patient's comfort.
3.
Guidance Techniques: Pericardiocentesis may be performed under the guidance of imaging
techniques, including echocardiography or fluoroscopy. These aid in accurate
needle placement, enhancing the safety and efficacy of the procedure.
4.
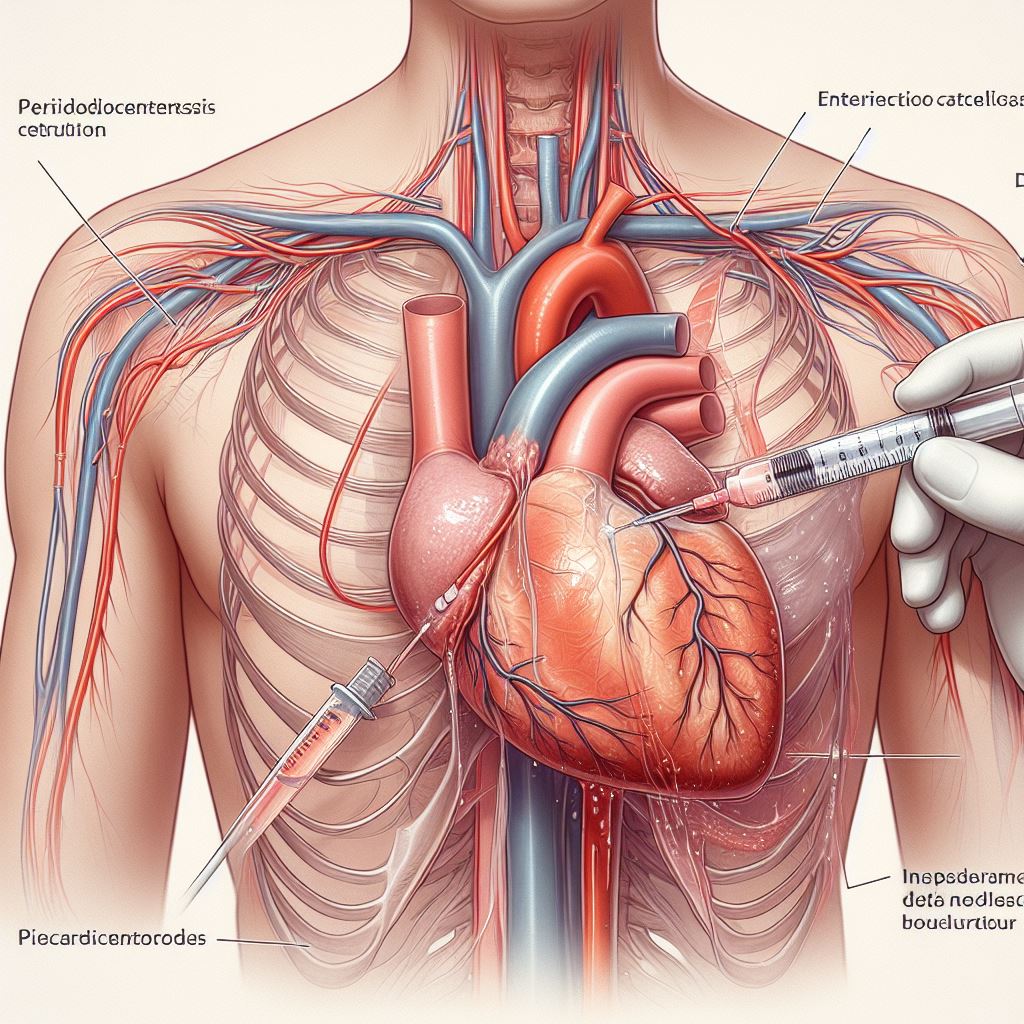
Needle Insertion: A specialized needle is carefully inserted through the chest wall into
the pericardial sac, guided by the imaging modality chosen. This precise
insertion is critical to avoid complications.
5.
Fluid Drainage: Once the needle is appropriately positioned, excess fluid is aspirated,
relieving pressure within the pericardium. The amount of fluid drained depends
on the severity of the effusion.
6.
Monitoring: Continuous
monitoring, encompassing electrocardiography and blood pressure measurement, is
crucial throughout the procedure to detect any potential complications
promptly.
Risks and Benefits: Benefits:
1.
Symptom Relief: Pericardiocentesis offers rapid relief from symptoms associated with
pericardial effusion, such as chest pain, shortness of breath, and general
discomfort.
2.
Diagnostic Insight: Beyond symptom relief, the procedure allows for the analysis of
pericardial fluid, aiding in the identification of the underlying cause,
whether infectious, inflammatory, or neoplastic.
3.
Prevention of Complications: By promptly draining excess fluid, pericardiocentesis helps prevent
complications like cardiac tamponade, ensuring the heart can function
optimally.
Risks:
1.
Bleeding: There is a risk of
bleeding, particularly in patients on anticoagulant medications. Close
monitoring during and after the procedure is crucial to manage this risk
effectively.
2.
Infection: As with any
invasive procedure, there is a potential risk of infection. Stringent sterile
techniques are employed to minimize this risk.
3.
Arrhythmias: The procedure may induce heart rhythm disturbances, although this risk
is relatively low and is closely monitored during the intervention.
4.
Perforation: In rare instances, inadvertent injury to the heart or adjacent blood
vessels may occur. The use of imaging guidance minimizes this risk, and experienced
healthcare professionals ensure a high level of safety.
Recovery and Outlook: Recovery:
1.
Observation: Post-procedure, patients are typically observed for a few hours to
monitor for any immediate complications or adverse reactions.
2.
Pain Management: Pain at the insertion site is managed with appropriate pain
medications, ensuring the patient's comfort during the recovery phase.
3.
Follow-up: Follow-up
appointments are scheduled to monitor the patient's recovery progress and
address any concerns or questions they may have.
Outlook: The overall
outlook after pericardiocentesis is generally positive, with most patients
experiencing significant relief from symptoms. The success of the procedure is
contingent on various factors, including the underlying cause of pericardial
effusion and the patient's overall health. Continuous monitoring and follow-up
care are essential components of ensuring a favorable long-term outlook.