Coronary Angiography
Coronary Angioplasty, also referred to as Percutaneous Coronary Intervention (PCI) or balloon angioplasty, is a minimally invasive procedure designed to address blocked or narrowed coronary arteries. These arteries play a pivotal role in supplying blood to the heart muscle, and when obstruction occurs due to plaque buildup, it can lead to chest pain (angina) or, in severe cases, a heart attack. Coronary Angioplasty serves as a vital tool to restore blood flow, alleviate symptoms, and prevent further cardiovascular damage.
Why it's done
Coronary Angioplasty is employed for various medical reasons, including:
1. Relief of Angina: To alleviate chest pain or discomfort resulting from reduced blood flow to the heart muscle.
2. Treatment of Heart Attack: In emergency situations, angioplasty is a life-saving measure, opening blocked arteries during a heart attack to minimize damage to the heart muscle.
3. Improvement of Blood Flow: To enhance blood flow in coronary arteries compromised by atherosclerosis, a condition characterized by the accumulation of fatty deposits.
Risks
While Coronary Angioplasty is generally safe and effective, like any medical procedure, it is not without risks. Potential complications may include:
1. Bleeding: Occurring at the catheter insertion site.
2. Allergic Reaction: A rare response to the contrast dye used during the procedure.
3. Blood Vessel Damage: Possible harm during catheter insertion.
4. Infection: Risk of infection at the catheter insertion site.
5. Blood Clots: Formation, either at the stent site or elsewhere in the bloodstream.
It is crucial to understand that your healthcare team will thoroughly discuss these potential risks and benefits with you before proceeding with the procedure. This informed consent process ensures that you are aware of the potential outcomes and can actively participate in your healthcare decisions.
How you prepare
Preparation for Coronary Angioplasty involves several key steps, including:
1. Fasting: Patients are often instructed not to eat or drink for a specific period before the procedure.
2. Medication Management: Adjustments to regular medications, especially blood thinners, may be necessary.
3. Medical History: Provide a detailed account of your medical history and any known allergies to ensure a safe procedure.
This preparatory phase is vital in ensuring the success and safety of the Coronary Angioplasty.
During the procedure
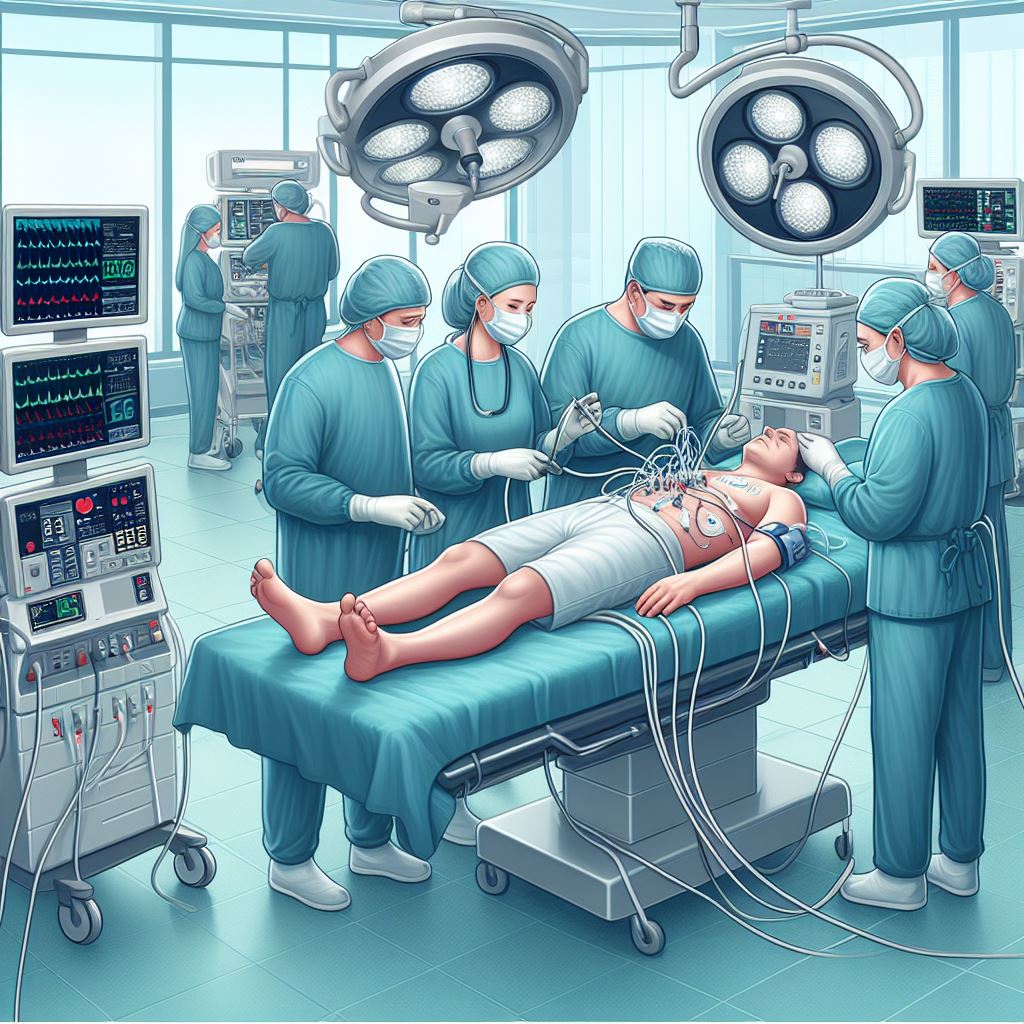
Coronary Angioplasty is typically performed in a specialized catheterization laboratory. Here's an overview of the procedural steps:
1. Anesthesia: Local anesthesia is administered to numb the catheter insertion site, usually in the groin or wrist.
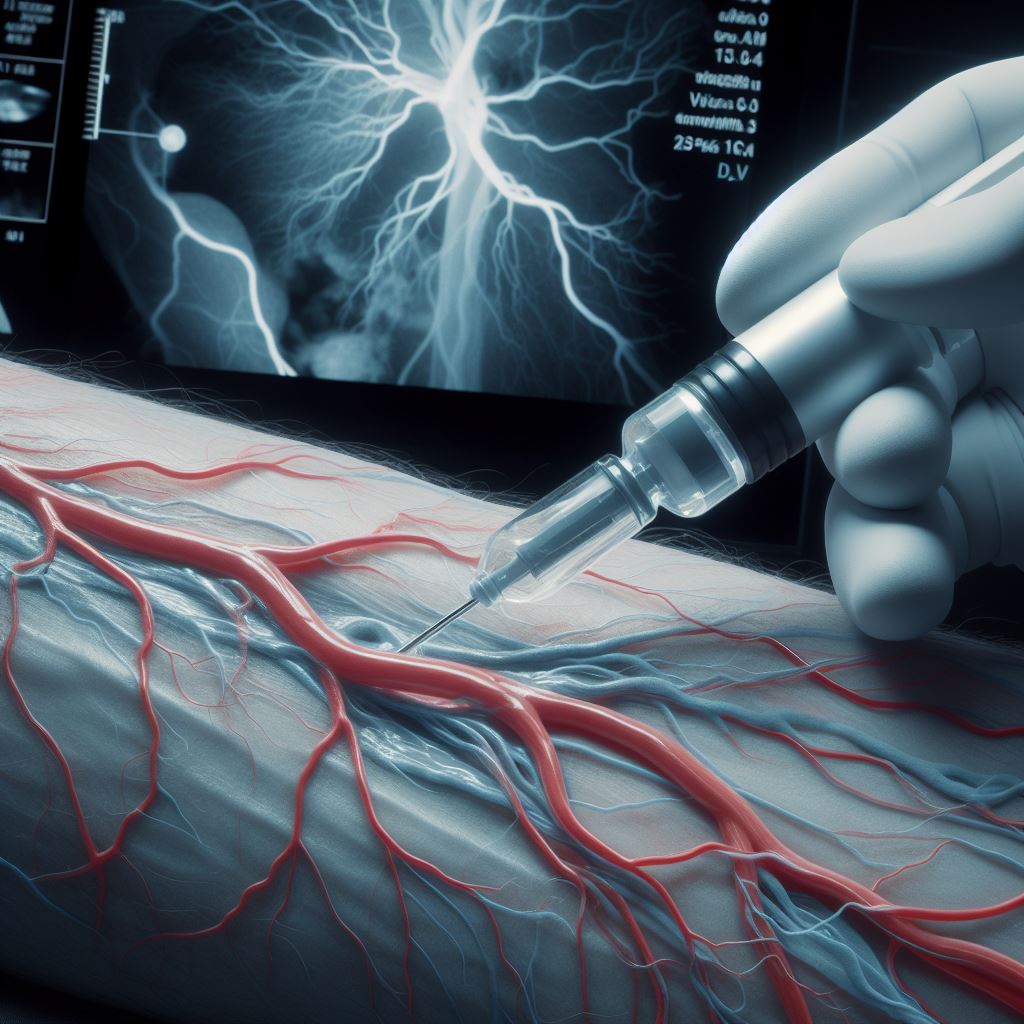
2. Catheter Insertion: A thin, flexible tube (catheter) is threaded through blood vessels to the coronary arteries.
3. Contrast Dye Injection: Contrast dye is injected through the catheter, allowing the physician to visualize the coronary arteries on X-ray images.
4. Balloon Inflation: A small balloon at the tip of the catheter is inflated to compress the plaque and widen the narrowed artery.
5. Stent Placement: In some cases, a stent (a small mesh tube) is inserted and expanded to support the artery and prevent future blockages.
6. Monitoring: Throughout the procedure, the medical team monitors your heart rate, blood pressure, and other vital signs.
After the procedure
Recovery from Coronary Angioplasty involves several key elements:
1. Monitoring: After the procedure, you'll be closely monitored in a recovery area to ensure stability.
2. Medication: Prescription of medications, including antiplatelet drugs, to prevent blood clots and manage various aspects of heart health.
3. Catheter Removal: The catheter is removed, and pressure is applied to the insertion site to prevent bleeding.
Patients are encouraged to communicate any discomfort or concerns to the healthcare team during this recovery period.
Results
The outcomes of Coronary Angioplasty are often immediate and can lead to significant improvements in heart health. These may include:
1. Symptom Relief: Immediate relief from chest pain or angina.
2. Improved Exercise Tolerance: Enhanced ability to engage in physical activities without discomfort.
3. Reduced Risk of Future Events: Lowered risk of future heart attacks and cardiovascular events.
Your healthcare team will provide you with detailed information about the success of the procedure and offer guidance on post-procedure care. Additionally, lifestyle modifications and medications may be recommended to support ongoing heart health.
Post-Procedure Care
After Coronary Angioplasty, a comprehensive approach to post-procedure care is crucial. This includes:
1. Medication Adherence: It is essential to adhere to prescribed medications, such as antiplatelet drugs and cholesterol-lowering medications, to prevent complications.
2. Follow-up Appointments: Regular follow-up appointments with your healthcare provider are scheduled to monitor your progress and address any concerns.
3. Lifestyle Modifications: Adopting heart-healthy lifestyle changes, including a balanced diet, regular exercise, smoking cessation, and stress management.
Your healthcare team will work collaboratively with you to create a personalized plan tailored to your specific needs and circumstances.