Peripheral Angioplasty
Peripheral Angioplasty: A Comprehensive Exploration of Restoring Peripheral Arterial Health
Welcome to our detailed exploration
of Peripheral Angioplasty, a sophisticated medical procedure designed to
restore blood flow in the peripheral arteries. Our expert medical team is here
to provide an in-depth understanding of why this procedure is performed,
potential risks, preparations before and after the surgery, the outlook for
patients, and alternative options available.
Why Peripheral Angioplasty?
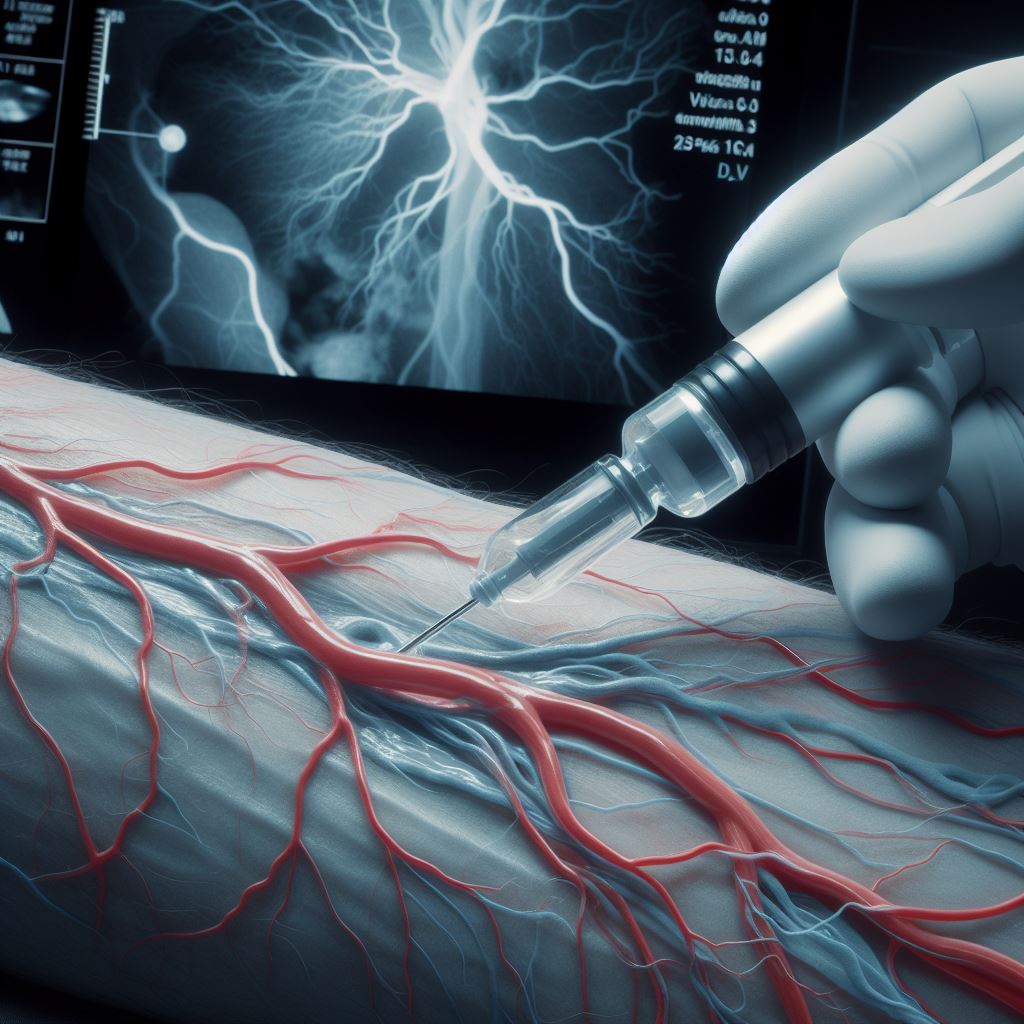
Peripheral Angioplasty is a crucial intervention for individuals
grappling with Peripheral Artery Disease (PAD). PAD occurs when arteries
outside the heart and brain narrow or become blocked, often due to the buildup
of plaque. This procedure is aimed at opening these narrowed or blocked
arteries, thereby improving blood circulation and alleviating symptoms such as
leg pain, cramping, and numbness.
1. Symptomatic PAD: Peripheral Angioplasty is often recommended for individuals
experiencing symptoms during physical activity, such as pain or discomfort in
the legs. This can significantly enhance the patient's ability to engage in
daily activities.
2. Non-healing Wounds: In cases where PAD leads to non-healing wounds or ulcers in the legs,
Peripheral Angioplasty can promote better blood flow, aiding in the healing
process and preventing further complications.
3. Preventing Amputation: In severe cases, especially those at risk of amputation due to Critical
Limb Ischemia, Peripheral Angioplasty becomes a critical intervention to save
limbs and improve overall quality of life.
Risks Associated with Peripheral
Angioplasty:
While Peripheral Angioplasty is generally considered safe, it's
imperative to be aware of potential risks and complications. A thorough
discussion with the healthcare team before the procedure is crucial to ensure
informed consent. Potential risks include:
1. Bleeding at the Catheter Insertion Site: The insertion of catheters into blood vessels carries a risk of
bleeding. However, this is typically minimal and can be managed effectively.
2. Blood Vessel Damage: There's a slight risk of damage to blood vessels during the procedure.
This risk is carefully mitigated through the expertise of the medical team.
3. Infection: Although rare, there is a potential risk of infection, especially at
the catheter insertion site. Strict sterile procedures are followed to minimize
this risk.
4. Allergic Reaction to Contrast Dye: Contrast dye is often used during angioplasty procedures to enhance
imaging. While allergic reactions are rare, they can be managed with
appropriate medical intervention.
5. Restenosis: There's a possibility of the treated artery re-narrowing over time.
This may require additional interventions or close monitoring.
Before the Procedure:
A successful Peripheral Angioplasty requires careful preparation to
ensure the best possible outcomes. Pre-procedural preparations include:
1. Medical Evaluation: A thorough medical evaluation, including imaging studies, will be
conducted to assess the extent and location of arterial blockages.
2. Medication Review: It's essential to inform your healthcare team about any medications you
are taking, as some may need to be adjusted or temporarily discontinued before
the procedure.
3. Fasting: Depending on the
type of anesthesia used, you may be required to fast for a specific period
before the procedure.
After the Procedure:
Post-procedural care is crucial to ensure a smooth recovery and minimize
complications. Key aspects of post-procedural care include:
1. Monitoring: After the procedure, you will be closely monitored for a brief period
to ensure stability and detect any immediate complications.
2. Medication: Medications may be prescribed to prevent blood clots and manage pain or
discomfort. It's essential to follow the prescribed medication regimen
diligently.
3. Recovery Plan: A personalized recovery plan will be provided, including instructions
for physical activity, wound care (if applicable), and follow-up appointments.
Adhering to this plan is vital for long-term success.
Outlook:
Peripheral Angioplasty often yields significant improvements in symptoms
and overall quality of life. However, the long-term success of the procedure
depends on several factors, including:
1. Lifestyle Changes: Adopting a healthy lifestyle, including maintaining a balanced diet and
regular exercise, is crucial for long-term success.
2. Medication Adherence: Strict adherence to prescribed medications, such as antiplatelet drugs
and cholesterol-lowering medications, is essential for preventing
complications.
3. Managing Risk Factors: Controlling risk factors such as diabetes, hypertension, and smoking is
imperative for maintaining vascular health.
Alternatives to Peripheral
Angioplasty:
While Peripheral Angioplasty is a highly effective intervention,
alternative options may be considered based on individual circumstances. These
alternatives include:
1. Medication Management: In some cases, medications alone may be sufficient to manage symptoms
and slow the progression of PAD.
2. Lifestyle Modifications: Adopting a healthier lifestyle, including quitting smoking, regular
exercise, and a heart-healthy diet, can positively impact vascular health.
3. Surgical Interventions: In cases where angioplasty may not be suitable, surgical interventions
such as bypass surgery may be considered.
Our dedicated medical team is
committed to providing personalized care, ensuring the best possible outcomes
for patients undergoing Peripheral Angioplasty. If you have any questions or
concerns, we encourage you to reach out to us for further information and
support.